Case ReportLung/Thoracic Cancer
Chemoradiotherapy-induced toxicity with high-dose three-dimensional conformal radiotherapy for lung cancer
Images


CASE SUMMARY
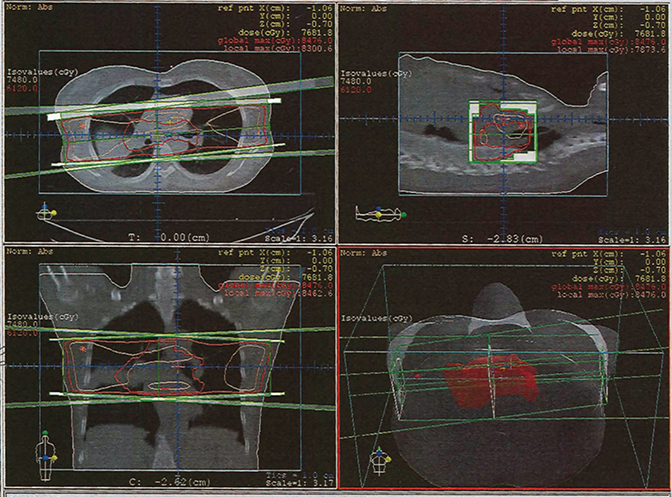
A 58-year-old African-American woman presented with a slowly enlarging, inferior right upper lobe ground-glass opacity (2.8 cm) for which biopsy proved well-differentiated adenocarcinoma of lung origin. Seven years earlier, the patient had undergone concurrent chemoradiotherapy at an outside institution for a stage IIIA adenocarcinoma of the right middle lobe. She had received weekly carboplatin/paclitaxel with concurrent radiation prescribed to 74 Gy using a 3-dimensional conformal radiotherapy technique (3D-CRT). The arrangement employed 2 parallel-opposed, oblique fields (only a few degrees off laterals) for the entire course (Figure 1).
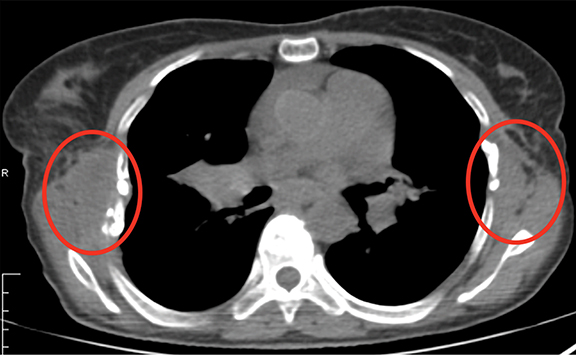
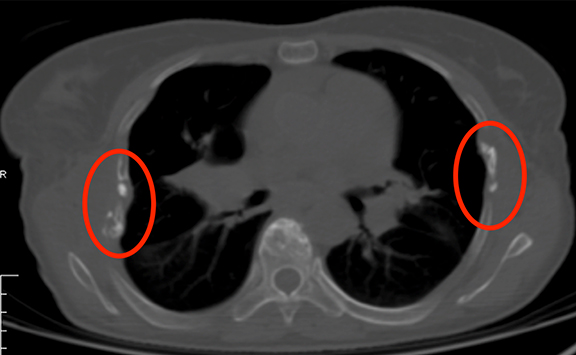
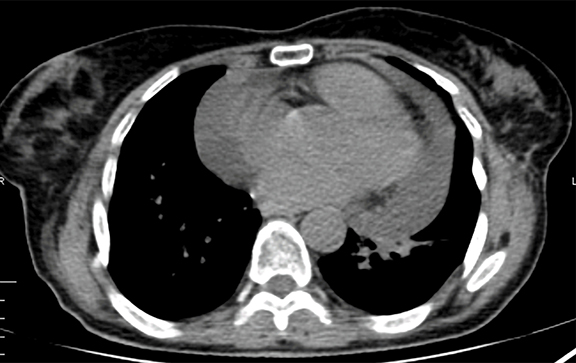
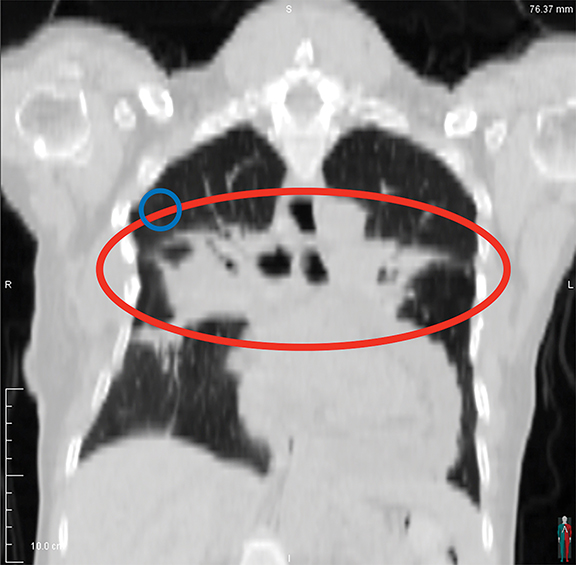
Upon re-presentation, she suffered from treatment-induced pulmonary fibrosis, chronic pericardial effusion, fractured ribs, chest wall fibrosis, and gastrostomy-tube dependent dysphagia (Figure 2). Because of the new lesion’s estimated abutment of the prior radiation’s superior field edge (Figure 2D) and her previous toxicity, the patient elected to undergo sublobar resection. Pulmonary function tests indicated only a mild restrictive pattern (FEV1-1.97L/73%;FVC-2.65L/82%;TLC-3.98L/79%). Surgery was relatively uncomplicated, but the patient suffered severe postoperative acute respiratory distress syndrome. This precipitated a complicated hospital course that ultimately led to death.
IMAGING FINDINGS
CT examination of the thorax at re-presentation demonstrated dramatic soft tissue changes corresponding to the previous radiation lateral field arrangement (Figures 1 and 2). Extraordinary bilateral rib fractures and chest wall fibrosis bracketed linear band-like pulmonary fibrosis traversing the patient’s chest as well as a moderate pericardial effusion.
DIAGNOSIS
Severe, late chemoradiotherapy-induced, lung, esophageal, heart, and chest wall toxicity, compounded by post-treatment surgical complications.
DISCUSSION
Radiation oncologists have a substantially increased workload in treatment planning and delivery when compared with the 2D and early 3D eras. Numerous treatment details and patient factors must be considered, and failure to do so can yield dramatic and unexpected toxicities. In particular, tumor and normal tissue delineation has become a labor of love, with contouring more akin to wielding the surgeon’s knife than the wax pencils of old. Physicians are then called upon to critically examine a variety of treatment criteria before selecting the “optimal” plan.
Rising concern focuses on chemoradiation-induced toxicities in treatment of locally advanced, nonsmall cell lung cancer (NSCLC). Publication of results from RTOG 0617 (randomized phase III comparison of standard-dose [60 Gy] vs high-dose [74 Gy] conformal radiotherapy with concurrent and consolidation carboplatin/paclitaxel ± cetuximab in patients with stage IIIA/IIIB NSCLC) has intensified uneasiness. Increased utilization of higher radiation doses, expansion of low-dose wash with intensity-modulated radiation therapy (IMRT), and potent radiosensitization with carboplatin/paclitaxel have each been implicated as contributors to treatment-induced morbidity/mortality.1-3
Recurrences and local failures in lung cancer remain common. Attempts to further intensify therapy have been met with mixed results. RTOG 0617 was initiated as a randomized, 2-by-2 factorial, phase III effort to investigate both the addition of cetuximab and dose escalation from 60 Gy to 74 Gy.1 Unfortunately, neither cetuximab nor dose escalation proved beneficial in this trial. Most disconcerting to radiation oncologists was the survival detriment in the 74 Gy arm, often attributed to treatment-related toxicity because no differences were noted in disease recurrence. On multivariate analysis, the prescription dose, maximal grade of esophagitis, planning target volume, heart V5, and heart V30 were each independent predictors of shorter overall survival.
When delivering such high doses of radiation therapy, IMRT is commonly employed to reduce dose to critical structures, such as the lung, heart, and esophagus. By using multiple computer-optimized and modulated fields, IMRT can achieve highly conformal dose distributions, with rapid fall-off toward nearby critical structures, that compare favorably with results from 3D-CRT.4 Quality of life (QoL) data from RTOG 0617 confirmed worse toxicity in the high-dose arm, but IMRT lessened clinically meaningful declines in QoL.5 It has been argued, however, that IMRT represents a double-edged sword, because it increases exposure of nearby normal tissue to a bath of lower doses (< 10 Gy). Healthy lung tissue may be particularly at risk.
The lung V20 first emerged as the most predictive marker for pneumonitis in early 3D-CRT approaches (APPA followed by parallel opposed obliques off-cord).6 With modern 3D-CRT/IMRT techniques, the entire dose–volume curve has increased in significance. Retrospective data from MD Anderson Cancer Center have posited that the V5, V25, V35, V45, and absolute volumes may each predict for radiation pneumonitis.7,8 Ultimately, balancing low- and high-dose conformality seems to produce optimal plans.9 Additional recently presented findings from RTOG 0617 suggest that IMRT reduces rates of clinically significant pneumonitis despite increased integral dose.10 Multiple published IMRT clinical experiences, reporting reasonable rates of toxicity, are reassuring,7,8 In the patient presented, a comparative IMRT plan was generated but rejected in favor of 3D-CRT.
In this case, 3D-CRT was nominally utilized, although the resultant plan is relatively non-“conformal.” The dose-volume histogram (DVH) in Figure 3 accompanied the treatment fields. The delivered plan possessed a lower V5 and V20 than the comparison IMRT plan (unavailable). However, the lateral fields resulted in large hotspots in normal lung, chest wall, heart, and esophagus, with a maximum point dose of 84.76 Gy (~115%) (Figure 1). The IMRT plan had a similar V5 and V20, raising concern that the number of fields employed may have been similarly few and not thoughtfully oriented. Despite the superficial appearance of 3D-CRT dosimetric superiority in this case, selection of this plan was misguided.
In addition, the heart, esophagus, and bilateral chest walls in this relatively young patient demonstrated life-altering toxicity: feeding-tube dependence for 7 years; multiple rib fractures/chest wall fibrosis; and chronic pericardial effusions. Only one of these structures (heart) was contoured. With either forward or inverse planning techniques, the ideal radiation therapy plan can be achieved only with thorough and thoughtful contour delineation. Optimal technique selection in modern planning is built on a foundation of accurate, reproducible volumes.
CONCLUSION
This case serves as a potent reminder that radiation oncologists must be diligent in contouring and plan evaluation. Beam arrangement, radiotherapy dose, conformality, modulation complexity, homogeneity, patient-specific features, and chemotherapeutic regimen (among others) must be examined. IMRT remains a viable and useful approach in the appropriate clinical setting. It should be noted that, despite initial stage IIIA disease, the patient had a durable response to initial chemoradiotherapy—but this came at a terrible cost.
REFERENCES
- Bradley JD, Paulus R, Komaki R, et al. Standard-dose versus high-dose conformal radiotherapy with concurrent and consolidation carboplatin plus paclitaxel with or without cetuximab for patients with stage IIIA or IIIB non-small-cell lung cancer (RTOG 0617): a randomised, two-by-two factorial phase 3 study. Lancet Oncol. 2015;16:187-199.
- Allen AM, Czerminska M, Jänne PA, et al. Fatal pneumonitis associated with intensity-modulated radiation therapy for mesothelioma. Int J Radiat Oncol Biol Phys. 2006;65:640-645.
- Wang L, Wu S, Ou G, et al. Randomized phase II study of concurrent cisplatin/etoposide or paclitaxel/carboplatin and thoracic radiotherapy in patients with stage III non-small cell lung cancer. Lung Cancer. 2012;77:89-96.
- Liu HH, Wang X, Dong L, et al. Feasibility of sparing lung and other thoracic structures with intensity-modulated radiotherapy for non-small-cell lung cancer. Int J Radiat Oncol Biol Phys. 2004;58:1268-1279.
- Movsas B, Hu C, Sloan J, et al. Quality of life analysis of a radiation dose-escalation study of patients with non-small-cell lung cancer: a secondary analysis of the Radiation Therapy Oncology Group 0617 randomized clinical trial. JAMA Oncol. 2016;2:359-367.
- Graham MV, Purdy JA, Emami B, et al. Clinical dose-volume histogram analysis for pneumonitis after 3D treatment for non-small cell lung cancer (NSCLC). Int J Radiat Oncol Biol Phys. 1999;45:323-329.
- Yom SS, Liao Z, Liu HH, et al. Initial evaluation of treatment-related pneumonitis in advanced-stage non-small-cell lung cancer patients treated with concurrent chemotherapy and intensity-modulated radiotherapy. Int J Radiat Oncol Biol Phys. 2007;68:94-102.
- Rice DC, Smythe WR, Liao Z, et al. Dose-dependent pulmonary toxicity after postoperative intensity-modulated radiotherapy for malignant pleural mesothelioma. Int J Radiat Oncol Biol Phys. 2007;69:350-357.
- Khalil AA, Hoffmann L, Moeller DS, et al. New dose constraint reduces radiation-induced fatal pneumonitis in locally advanced non-small cell lung cancer patients treated with intensity-modulated radiotherapy. Acta Oncol. 2015;54:1343-1349.
- Chun SG, Hu C, Choy H, et al. Comparison of 3-D conformal and intensity modulated radiation therapy outcomes for locally advanced non-small cell lung cancer in NRG Oncology/RTOG 0617 [abstract]. Int J Radiat Oncol Biol Phys. 2015;93:S1-S2.
Citation
Snider, JW III, Diwanji T, Amin P, Feigenberg SJ. Chemoradiotherapy-induced toxicity with high-dose three-dimensional conformal radiotherapy for lung cancer. Appl Rad Oncol. 2016;(2):28-31.
June 4, 2016
