Radiotherapy, including internal mammary nodal irradiation, and heart failure in patients receiving concurrent treatment with tr
Images
Abstract
The impact of radiation therapy (RT), including internal mammary nodal (IMN) RT on cardiac function in patients receiving concurrent treatment with trastuzumab, was studied.
Patients and Methods: Thirty-seven patients with stage I–III human epidermal growth factor-2 (HER2)–positive breast cancer treated with trastuzumab with or without concurrent RT met inclusion criteria. Changes in left ventricular ejection fraction (LVEF) were measured using multigated acquisition scans. The primary endpoint was heart failure (HF), defined as a ≥ 16% decrease in LVEF from baseline or a ≥ 10% decrease of baseline LVEF if this fell below 50%.
Results: HF incidence among the entire group of patients treated with trastuzumab was 24.3%. Of these HF cases, 55.6% were reversible within 1 year of trastuzumab initiation. Of those receiving RT, 28.1% had HF; of the group who did not receive RT, none had HF. Of patients treated with left-sided RT, 26.7% developed HF compared with 27.8% treated with right-sided RT. Of patients treated with IMN RT, 22.2% had HF compared to 30.4% who did not receive IMN RT. Eighty-nine percent of patients who developed HF received anthracycline-based chemotherapy compared to 54% who developed HF without anthracyclines.
Conclusion: Concurrent RT and trastuzumab administration was not found to significantly increase the risk of HF. No significant differences in incidence of HF by tumor laterality or IMN RT were noted. Age, race, and comorbidities did not correlate with increased HF risk; however, there was a strong trend toward an increasing risk of HF among patients receiving anthracycline-based chemotherapy.
Human epidermal growth factor receptor-2 (HER2) overexpression occurs in approximately 25% to 30% of all breast cancers and is associated with aggressive tumor growth and poor treatment outcomes. The development of trastuzumab, a recombinant monoclonal antibody that targets the extracellular domain of the HER2/neu receptor, has dramatically improved outcomes for this subset of breast cancer patients.1 With the use of trastuzumab, outcomes are similar to those seen in patients with HER2-negative disease.2-4
The most prominent adverse effect of trastuzumab is cardiac toxicity, with up to 25% of patients developing trastuzumab-mediated cardiomyopathy, defined as a significant decline in left ventricular ejection fraction (LVEF). Accompanying signs and symptoms of congestive heart failure (CHF) in certain instances necessitate discontinuation of the drug.5 Although the mechanisms by which trastuzumab induces cardiomyopathy are unknown, its effects on cardiac function tend to be reversible.6
In a similar fashion, radiation therapy (RT) has been shown to significantly reduce disease recurrence in early and locally advanced disease. This increase in local control has also improved overall survival.7 Although the cardiotoxic effects of RT have been well-documented, the majority of these effects were documented decades ago in an era of older techniques now largely obsolete.8
The mechanisms by which cardiac damage occurs following radiation are not fully understood. Current theories propose that high doses of radiation received by small volumes of the heart and coronary vessels induce atherosclerosis, predisposing patients to coronary events. In contrast, low-dose exposure to the entire heart is believed to cause microvascular damage and fibrosis, precipitating CHF.9 In a recent large national longitudinal study, Darby et al suggested that there may be no safe threshold below which damage is averted and that every 1 Gy increase in mean cardiac dose is associated with a 7.4% relative increase in the rate of major coronary events. 10
Two recent major cooperative group studies suggest a substantial benefit to nodal irradiation that includes treatment of the internal mammary nodal (IMN) chain. 11,12 Such data will likely increase the use of IMN RT, with a resultant increase in mean heart RT dose from 2-4 Gy to 10 Gy.13 This study was designed to examine in greater detail the techniques of RT used in a HER2-targeted subset of patients treated at a single institution, specifically examining the impact on cardiac function of concurrent treatment with RT and the known cardiotoxic systemic agent trastuzumab.
Patients and Methods
All breast cancer patients treated with trastuzumab with curative intent at the University of Maryland Marlene and Stewart Greenebaum Cancer Center between January 2000 and June 2011 were reviewed. This retrospective review was approved by the University of Maryland Institutional Review Board. During this time frame, patients were uniformly monitored for cardiotoxicity using multigated acquisition (MUGA) scans by a single medical oncologist. Each patient’s LVEF, as reported by the MUGA scan, was measured prior to initiation of treatment with trastuzumab. Subsequent MUGA scans occurred at 3, 6, 9, and 12 months after initiation of trastuzumab.
To be included in this study, patients must have been: (1) diagnosed with HER2-positive (by immunohistochemistry or by fluorescence in situ hybridization) breast cancer; (2) diagnosed with stage I, II, or III disease; (3) treated with curative intent; (4) without treatment with thoracic RT previously; and (5) recommended for and received trastuzumab alone or in concurrence with RT at the University of Maryland Marlene and Stewart Greenebaum Cancer Center. Trastuzumab was administered at an 8 mg/kg loading dose followed by 6 mg/kg every 3 weeks for 16 or 17 doses or at a 4 mg/kg loading dose followed by 2 mg/kg weekly for 52 doses. The trastuzumab treatment regimen was selected according to the medical oncologist’s preference. Patients with metastatic disease were purposely excluded.
The primary endpoint was heart failure (HF), defined as a ≥ 16% decrease in LVEF from baseline or a ≥ 10% decrease from baseline LVEF if falling below 50%. This definition is consistent with the criteria for discontinuation of trastuzumab from the prescriber manual.14 To determine whether the dose of radiation to the heart contributed to HF, tumor laterality (ie, right- vs. left-sided RT) and employment of IMN RT were selected as statistical parameters. Cardiac RT dose is, of course, regularly higher for women with left-sided cancers, with the highest doses experienced when the IMN chain is targeted.15 Data were also collected on each patient’s age, race, tumor type, tumor grade, stage (TNM), chemotherapy regimen, and history of comorbidities (including diabetes mellitus, hypertension, hyperlipidemia, coronary artery disease, and smoking).
Incidences of HF in the RT vs. no RT group, left- vs. right-sided RT, IMN vs. no IMN RT, and left- vs. right-sided IMN RT were assessed using the Z-test with statistical significance threshold of P ≤ 0.05 in a 2-tailed analysis. Patients were also stratified by whether or not they were subsequently diagnosed with HF. Baseline characteristics were compared between the HF vs. no HF group using the Z-test. Patients meeting criteria for HF were considered to have reversible HF if their LVEF recovered following initial decrease below the predetermined thresholds.
Data were also collected on each patient to determine whether a major coronary event occurred during a median follow-up period of 5 years after treatment with RT. A major coronary event was defined per Darby et al as the occurrence of a myocardial infarction, coronary revascularization, or death from ischemic heart disease.10
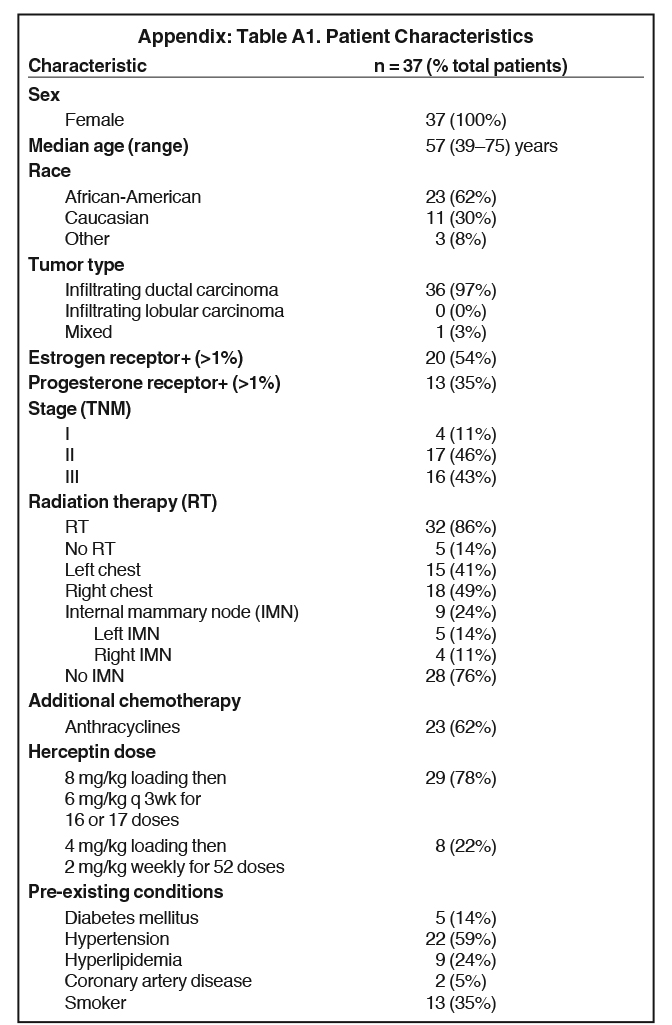
Thirty-seven women with stage I–III breast cancer met the inclusion criteria (see Appendix Table A1 for patient characteristics). Of these patients, 32 were treated concurrently with RT, 15 patients were treated to the left, and 18 to the right. IMNs were targeted in 9 patients; 5 patients of whom received left-sided RT, and 4 of whom received right-sided RT. Five patients were treated with trastuzumab alone.
Results
A total of 130 radionuclide ventriculograms were performed during the study period. All patients underwent baseline imaging, 19 patients underwent imaging at 3 months following treatment, 28 at 6 months, 26 at 9 months, and 20 at 12 months. Four patients underwent MUGA scans at all five time points.
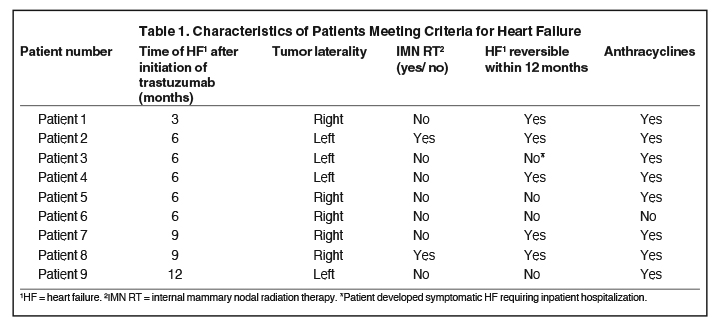
Based on LVEF as determined by MUGA scans, 9 patients met the criteria for HF (Table 1). All of these patients were treated concurrently with RT. Five of the 9 HF cases were reversible, ie, a MUGA scan acquired following the initial scan in which HF was detected but within 12 months after the start of trastuzumab, showed recovery of cardiac function above threshold. The remaining 4 patients who met criteria for HF did not achieve recovery of function above threshold within the 12-month period after initiation of treatment with trastuzumab. One of the 4 patients developed symptomatic HF requiring discontinuation of treatment with trastuzumab and inpatient hospitalization. Prior to ending treatment, the patient received a lumpectomy and 6 cycles of trastuzumab.
Twenty-eight percent of the patients (9/32) treated with RT developed HF; none of the 5 patients who did not undergo RT developed HF. Twenty-six percent of patients (4/15) who received left-sided RT developed HF compared to 28% of patients (5/18) who received right-sided RT. Twenty-two percent of patients (2/9) who had IMN RT developed HF compared to 30% of patients (7/23) who did not have IMN RT. Forty percent of patients (2/5) who received left-sided IMN RT developed HF; none of the 4 patients who received right-sided IMN RT developed HF.
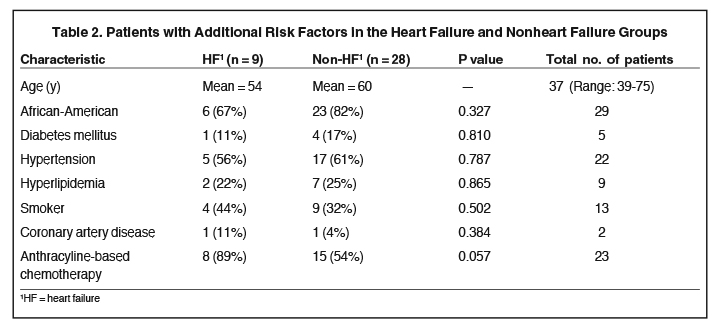
Patients’ comorbidities included diabetes mellitus, hypertension, hyperlipidemia, and coronary artery disease. No statistically significant difference was noted in the risk of HF based on these characteristics in this small series. Age, African-American race, and history of smoking also did not contribute to an increased risk of HF. However, 89% of patients (8/9) who developed HF had previously received anthracycline-based chemotherapy compared to 54% of non-HF patients (15/28) (Table 2).
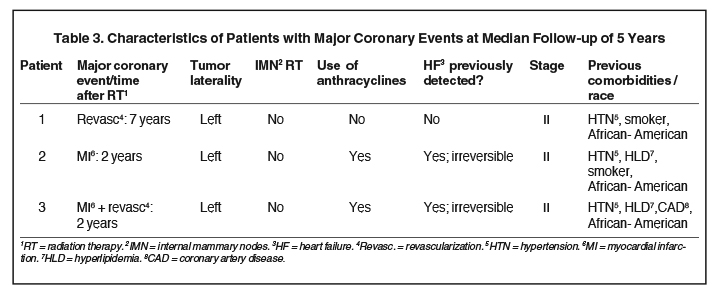
Each patient was further reviewed to determine whether a major coronary event occurred during a median follow-up of 5 years after completion of RT. Nine percent of patients (3/32) who received RT underwent a major coronary event (Table 3). None of the five patients (0/5) who did not receive RT had a major coronary event at a median follow-up of 5 years after treatment with trastuzumab alone.
Discussion
The cardiotoxic effects of treatment with trastuzumab have been well-established, whereas the additional impact of RT given concurrently with targeted HER2-based systemic therapy has been investigated in only a few series. The most comprehensive study performed to date involved assessment of 1,503 early stage, HER2-positive breast cancer patients. These patients were randomly assigned to different combinations of doxorubicin and cyclophosphamide, followed by weekly paclitaxel and later by trastuzumab. RT commenced within 5 weeks after paclitaxel, concurrently with trastuzumab. Results showed no significant increase in adverse or acute cardiac events associated with concurrent trastuzumab and RT after a median follow-up of 3.7 years. However, RT to the internal mammary lymph nodes was prohibited, so that the RT dose received by the heart was quite low.16
Additional smaller studies that assessed the combined effects of trastuzumab and RT have not found a significant increase in adverse events among patients receiving concurrent treatment. In one study in which skin and cardiac toxicities were evaluated in 57 patients receiving concurrent trastuzumab and RT, rates of abnormal LVEF and skin toxicity were deemed acceptable.17 IMN radiation, however, was not assessed. In two additional studies in which acute cardiotoxicity was evaluated in 106 patients and in 59 patients who received concurrent trastuzumab and RT, no excess cardiotoxicity was observed with RT, regardless of the side irradiated or the addition of IMN RT. 18,19
Our study further strengthens the small body of previous data that has failed to identify a causal link between concurrent trastuzumab/RT and subsequent HF. Unlike previous studies in which the incidence of cardiotoxicity was evaluated by quantifying LVEF using imprecise techniques, this study utilized a standardized, reproducible method at regular 3-month intervals in unselected patients. Moreover, previous studies may have underestimated the acute reversible effects on cardiac function from RT by using echocardiography, a less sensitive technique compared to the MUGA scans used in this study.20
Increasing Radiation Doses to the Heart as Measured by Tumor Laterality and IMN RT
The treatment of left-sided breast cancers with RT poses a risk of increasing cardiotoxicity.15 Darby et al found a dose-dependent increased risk of late ischemic heart disease associated with RT of the left breast.10 However, a recent large-scale clinical investigation showed that tumor laterality does not influence survival among breast cancer patients when treatment planning based on modern techniques, including computed tomography simulation, is utilized. In that study, 344,831 patients were followed for 10 years, and no difference in overall survival was noted by tumor laterality for patients treated for breast-only and breast-plus-regional-nodal RT. The authors, therefore, attributed Darby et al’s findings to the use of outdated radiation techniques.21
>The use of IMN RT in the treatment of breast cancer has remained controversial because of its potential to increase cardiac dose, with previous studies demonstrating no improvement in overall survival.22 Recent data from a study published in the New England Journal of Medicine suggests that IMN RT in patients with early stage breast cancer may actually contribute to a benefit in overall survival, also improving disease-free survival, distant disease-free survival, and breast cancer mortality. This trial randomized 4,004 stage I–III breast cancer patients, who had undergone either mastectomy or breast-conserving surgery and axillary dissection, to regional nodal irradiation or to no regional nodal irradiation. The primary endpoint was overall survival, and the data were published after a median follow-up of 10.9 years. In addition to improvement in overall survival, the authors found a low rate of heart disease and death from heart disease.11
The present study did not find an increase in the incidence of HF based on tumor laterality or IMN RT in the setting of concurrent trastuzumab therapy. This may be the result of care taken to minimize the amount of radiation received by the heart using modern treatment planning and breath-hold techniques.21,23 This also may be attributable to a bias toward treating patients with stronger baseline cardiac function with IMN RT. The small sample size of this study and the relatively short follow-up must also be considered; it is possible that a larger sample size followed over a longer period would have demonstrated a higher incidence of patients with HF. In general, early radiation-induced cardiac changes are believed to be detected as early as 6 months post-RT using single-photon emission computed tomography.24 However, late effects of thoracic radiation generally become evident 3-29 years after treatment.25
Use of Anthracycline-Based Chemotherapy and Additional Risk Factors
The efficacy of anthracyclines in the treatment of early breast cancer, irrespective of receptor status, has been proven in multiple large cohort trials and meta-analyses. 26 Moreover, the use of trastuzumab combined with an anthracycline regimen has shown a significant benefit in both disease-free and overall survival in patients with HER2-positive disease.2 However, the development of significant cardiotoxicity related to anthracyclines and the emergence of newer agents (such as taxanes), that appear to limit cardiotoxicity but with similar treatment efficacy, have called the use of anthracyclines into question.26
Our study demonstrates a trend toward an increase in HF among women treated with anthracycline-based treatment regimens. Future studies are needed to determine whether agents, such as taxanes, associated with less cardiotoxicity have equal anticancer efficacy in combination with trastuzumab. The newer agent pertuzumab, a humanized monoclonal antibody that targets a different domain of the HER2 receptor from that targeted by trastuzumab, should also be studied in combination with anthracyclines. Although limited, data suggest that when combined with trastuzumab, pertuzumab is well-tolerated, with LVEF remaining close to baseline.27
In addition to the use of anthracyclines, patient characteristics, such as age, race, and comorbidities, have been investigated as risk factors for developing HF in women treated with trastuzumab. One retrospective analysis conducted at the University of Maryland Medical Center, Baltimore, reported a higher risk of developing decreased LVEF in African-American women.20 Several studies have also identified an association between older age or a history of heart disease and trastuzumab-induced cardiotoxicity.28 The present study found no significant associations between age, race, history of previous heart disease, or history of smoking and treatment-induced cardiotoxicity.
Conclusions
In this single-institution experience, the concurrent use of RT did not appear to increase the risk of HF among patients receiving trastuzumab. Nor were increased radiation doses to the heart with left-sided radiation and/or targeting of the IMN chain found to be associated with an increased risk of HF. A strong trend toward an increasing risk of HF was identified in patients receiving anthracycline-based chemotherapy. Future studies are needed to confirm these findings in a larger sample size and with LVEF monitoring for periods ≥ 12 months. This could help determine whether there is a need to further lower radiation doses to the heart using more sophisticated radiation techniques such as proton therapy in women receiving systemic agents with known cardiotoxic effects.
References
- Ménard S, Pupa SM, Campiglio M, Tagliabue E. Biologic and therapeutic role of HER2 in cancer. Oncogene. 2003;22:6570-6578.
- Piccart-Gebhart MJ, Procter M, Leyland-Jones B, et al. Trastuzumab after adjuvant chemotherapy in HER2-positive breast cancer. N Engl J Med. 2005;353:1659-1672.
- Baselga J, Perez EA, Pienkowski T, Bell R. Adjuvant trastuzumab: a milestone in the treatment of HER-2-positive early breast cancer. Oncologist. 2006;11(suppl 1):4-12.
- Slamon D, Eiermann W, Robert N, et al. Adjuvant trastuzumab in HER2-positive breast cancer. N Engl J Med. 2011;365:1273-1283.
- Fallah-Rad N, Walker JR, Wassef A, et al. The utility of cardiac biomarkers, tissue velocity and strain imaging, and cardiac magnetic resonance imaging in predicting early left ventricular dysfunction in patients with human epidermal growth factor receptor II-positive breast cancer treated with adjuvant trastuzumab therapy. J Am Coll Cardiol. 2011;57:2263-2270.
- Ewer MS, Vooletich MT, Durand JB, et al. Reversibility of trastuzumab-related cardiotoxicity: new insights based on clinical course and response to medical treatment. J Clin Oncol. 2005;23:7820-7826.
- Darby S, McGale P, Correa C, et al. Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10,801 women in 17 randomised trials. Lancet. 2011;378:1707-1716.
- Senkus-Konefka E, Jassem J. Cardiovascular effects of breast cancer radiotherapy. Cancer Treat Rev. 2007;33:578-593.
- Stewart FA, Seemann I, Hoving S, Russell NS. Understanding radiation-induced cardiovascular damage and strategies for intervention. Clin Oncol (R Coll Radiol). 2013;25:617-624.
- Darby SC, Ewertz M, McGale P, et al. Risk of ischemic heart disease in women after radiotherapy for breast cancer. N Engl J Med. 2013;368:987-998.
- Poortmans PM, Collette S, Kirkove C, et al. Internal mammary and medial supraclavicular irradiation in breast cancer. N Engl J Med. 2015;373:317-327.
- Budach W, Kammers K, Boelke E, Matuschek C. Adjuvant radiotherapy of regional lymph nodes in breast cancer - a meta-analysis of randomized trials. Radiat Oncol. 2013;8:267.
- Jagsi R, Pierce L. Radiation therapy to the internal mammary nodal region in breast cancer: the debate continues. Int J Radiat Oncol Biol Phys. 2013;86:813-815.
- Genetech. Herceptin [trastuzumab]: highlights of prescribing information. South San Francisco, GA; Genetech; 1998.
- Sardaro A, Petruzzelli MF, D’Errico MP, Grimaldi L, Pili G, Portaluri M. Radiationinduced cardiac damage in early left breast cancer patients: risk factors, biological mechanisms, radiobiology, and dosimetric constraints. Radiother Oncol. 2012;103:133-142.
- Halyard MY, Pisansky TM, Dueck AC, et al. Radiotherapy and adjuvant trastuzumab in operable breast cancer: tolerability and adverse event data from the NCCTG Phase III rTial N9831. J Clin Oncol. 2009;27:2638-2644.
- Kirova YM, Caussa L, Granger B, et al. [Monocentric evaluation of the skin and cardiac toxicities of the concomitant administration of trastuzumab and radiotherapy]. Cancer Radiother. 2009;13:276-280.
- Shaffer R, Tyldesley S, Rolles M, Chia S, Mohamed I. Acute cardiotoxicity with concurrent trastuzumab and radiotherapy including internal mammary chain nodes: a retrospective single-institution study. Radiother Oncol. 2009;90:122-126.
- Caussa L, Kirova YM, Gault N, et al. The acute skin and heart toxicity of a concurrent association of trastuzumab and locoregional breast radiotherapy including internal mammary chain: a single-institution study. Eur J Cancer. 2011;47:65-73.
- Baron KB, Brown JR, Heiss BL, et al. Trastuzumab-induced cardiomyopathy: incidence and associated risk factors in an inner-city population. J Card Fail. 2014;20:555-559.
- Rutter CE, Chagpar AB, Evans SB. Breast cancer laterality does not influence survival in a large modern cohort: implications for radiation-related cardiac mortality. Int J Radiat Oncol Biol Phys. 2014;90:329-334.
- Chen RC, Lin NU, Golshan M, Harris JR, Bellon JR. Internal mammary nodes in breast cancer: diagnosis and implications for patient management—a systematic review. J Clin Oncol. 2008;26:4981-4989.
- Edvardsson A, Nilsson MP, Amptoulach S, Ceberg S. Comparison of doses and NTCP to risk organs with enhanced inspiration gating and free breathing for left-sided breast cancer radiotherapy using the AAA algorithm. Radiat Oncol. 2015;10:84.
- Lawrence MV, Saynak M, Fried DV, et al. Assessing the impact of radiation-induced changes in soft tissue density/thickness on the study of radiation-induced perfusion changes in the lung and heart. Med Phys. 2012;39:7644-7649.
- Jaworski C, Mariani JA, Wheeler G, Kaye DM. Cardiac complications of thoracic irradiation. J Am Coll Cardiol. 2013;61:2319-2328.
- Greene J, Hennessy B. The role of anthracyclines in the treatment of early breast cancer. J Oncol Pharm Pract. 2015;21:201-212.
- Lenihan D, Suter T, Brammer M, Neate C, Ross G, Baselga J. Pooled analysis of cardiac safety in patients with cancer treated with pertuzumab. Ann Oncol. 2012;23:791-800.
- Onitilo AA, Engel JM, Stankowski RV. Cardiovascular toxicity associated with adjuvant trastuzumab therapy: prevalence, patient characteristics, and risk factors. Ther Adv Drug Saf. 2014;5:154-166.
Support for this project was received from the University of Maryland Medical Center Department of Radiation Oncology, and the University of Maryland School of Medicine Office of Student Research.
Citation
Katz D, Snider JW, Patel K, Bentzen S, Nichols EM, Rosenblatt PY, Tkaczuk K, Feigenberg SJ. Radiotherapy, including internal mammary nodal irradiation, and heart failure in patients receiving concurrent treatment with tr. Appl Rad Oncol. 2016;(3):20-25.
September 12, 2016
