Speedy delivery makes rotational IMRT the technique of choice
Images
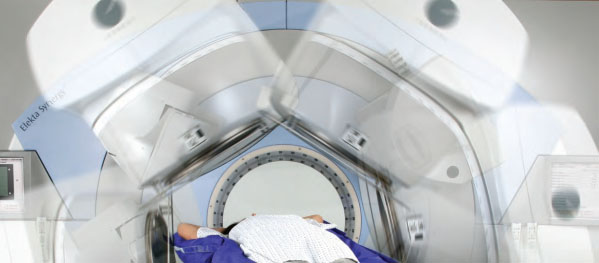
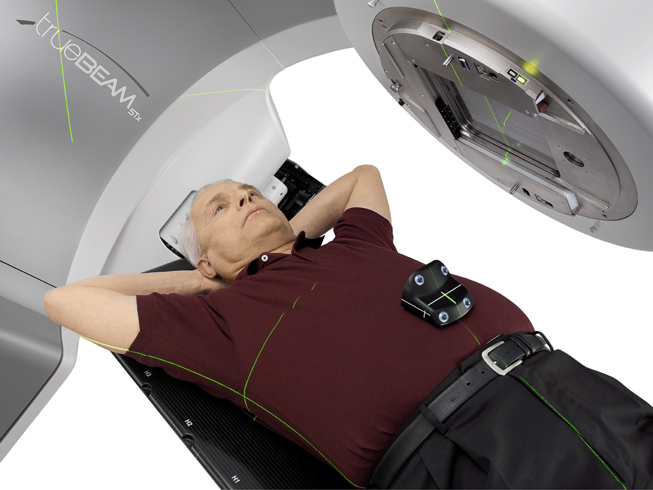
Intensity-modulated radiation therapy (IMRT) has become the method of choice for treating complex-shaped planning target volumes (PTV).1 During the last few years, rotational IMRT (rIMRT) techniques, such as volumetric-modulated arc therapy (VMAT) and helical tomotherapy have become widely available, delivering similar or better-quality treatments compared to conventional fixed-field IMRT (cIMRT).
Several studies have compared rIMRT techniques to helical tomotherapy and cIMRT. These comparisons focus on treatment plan quality based on satisfying target coverage while respecting defined organs-at-risk (OAR) criteria, target dose homogeneity, and treatment delivery efficiency.1 What sets rIMRT apart from helical tomotherapy and cIMRT are the faster treatment times.
Need for speed
Radiation oncology centers worldwide have implemented the VMAT technique using the following systems, RapidArc™ and TrueBeam™ by Varian Medical (Palo Alto, CA); the VMAT™ system by Elekta (Stockholm, Sweden); or the Smart-ArcTM, a module for VMAT available on the Pinnacle3 treatment planning solution from Philips Healthcare (Andover, MA). The distinguishing feature of these rIMRT systems is the treatment delivery time, which is much faster than that of cIMRT. In VMAT delivery, both dose rate and gantry rotation speed can vary, and these additional degrees-of-freedom increase the capability of beam intensity modulation.2
“The advantages of reduced treatment time are a reduction in interfraction motion, improvement in patient comfort, and an increase in patient throughput,” noted Jonas D. Fontenot, PhD, Adjunct Assistant Professor of Physics, Department of Physics, Mary Bird Perkins Cancer Center, Baton Rouge, LA.
The Mary Bird Perkins facility was an early adopter of Elekta’s VMAT system, initiating its VMAT program in mid-2009. Today, doctors treat all of the conditions that can be treated with cIMRT, including prostate, head and neck, lung, and brain and spinal cord cancers. In the last 18 months, they have started to use VMAT for lung stereotactic body radiation therapy (SBRT).
“SBRT is a hot topic in radiation oncology right now, and we are finding a lot of applications for VMAT. It has almost completely replaced cIMRT at our center,” said Fontenot.
Fontenot explains that the quality of the dose distribution that the patient receives with a VMAT plan is comparable to cIMRT. “It is not a matter of improving the dose received by the patient; however, the real benefit is the efficiency with which the treatments can be delivered. Studies from our group and others have shown that VMAT treatments can be delivered in 1/3 of the time as a cIMRT plan,” he said.
“If we were treating a patient with prostate cancer with cIMRT, we would probably need to use 7 or 9 fields, and a plan like that would take approximately 9 or 10 minutes to deliver. Contrast that with VMAT, where we can deliver the same quality treatment in a single arc that takes about 1-and-a-half minutes to deliver (Figure 1). Comparatively speaking, it’s quite a bit faster, which has several advantages.”
The University of Alabama at Birmingham radiation oncology program, which works with Varian’s RapidArc system as well as the TrueBeam platform, was looking to broaden its SBRT program and to do hypofractionated frameless stereotactic radiosurgery (SRS).
“The linacs can expand our SBRT program. They enable single and multifraction, hypofractionated frameless SRS treatments, offer better image-guidance over time, and more provide efficient treatments elsewhere in the body. We acquired the TrueBeam system for its efficient administration of SRS,” explained John B. Fiveash, MD, Radiation Oncologist, Department of Radiation Oncology, Associate Professor and Vice Chairman for Academic Programs, University of Alabama at Birmingham.
Designed for image-guided radiotherapy and radiosurgery, TrueBeam is a fully-integrated system designed from the ground up to treat moving targets at higher treatment delivery speeds with a dose delivery rate of up to 2,400 monitor units per minute. The system improves precision through better synchronization between imaging, patient positioning, motion management, beam shaping, and dose delivery technologies by performing accuracy checks every 10 milliseconds throughout an entire treatment.
“The greatest savings is in higher dose-per-fraction cases,” said Dr. Fiveash. As he recalls, the amount of time spent on a very-high-dose treatment for lung or liver surgery used to take 60 to 90 minutes. Today, with TrueBeam, they are scheduling high dose-per-fraction treatments in 30-minute time slots.
For some anatomical sites, quicker treatments can lead to greater accuracy as patients are more comfortable and less likely to move during the therapy. In prostate cancer, for example, gas patterns or rectal or bladder filling can move the target on the organ, and faster treatments leave less time for error caused by movement (Figure 2).
“If you have treatments lasting 10 to 12 minutes, 25% of the patients will have motion of the prostate > 3 mm. If you have a treatment that lasts a minute or two, it’s about 5% or less. A quick treatment with RapidArc or flattening filter free mode (FFF), if you’re doing stereotactic treatments in particular, has the advantage of accuracy,” said Dr. Fiveash.
With the FFF mode, the number of beam pulses per second remains the same (360 pulses/second at the maximum dose rate); however, the absence of attenuation due to the metal filter results in higher photon dose in the central portion of the beam. This means that the same dose could be delivered up to 4 times faster for this energy.3
A recently published study found that the 6-MV flattening filter-free mode (6F) of the Varian TrueBeam enables faster dose delivery and shortens treatment time, which is especially beneficial for stereotactic radiosurgery.4
“You can combine RapidArc with FFF mode and can do beam time in < 5 minutes. For multiple targets, it’s a big time saver. If you are treating multiple tumors, like metastases, it could take 2 to 4 hours on a Gamma Knife, but we can do that in 15 minutes,” Dr. Fiveash indicated. “That allows you to do extremely fast treatments for SRT and SBRT, all in a conventional time slot or 2 times lots. As a result, you can treat 4 to 5 patients in an hour.”
The ability to use the FFF mode on the TrueBeam system (Figure 2) is an important feature for doctors at UCSD Moores Cancer Center, La Jolla, CA. “I was excited about getting TrueBeam because of speed, the quality of the on-board imaging, and because it has the whole FFF technology,” said Arno J. Mundt, MD, Professor and Chair at UCSD Moores Cancer Center, La Jolla, CA.
The actual beam-on time for treating prostate cancer has dropped to 60 seconds. “The total time at a minimum would be 3 minutes—that includes going from one fixed-beam position to the next. RapidArc is much faster compared to static IMRT, which had a beam-on time of 3 to 5 minutes. And now it’s 60 seconds. It is a significant improvement in speed,” pointed out Todd Pawlicki, PhD, Director of Medical Physics at UCSD. “If you have more complicated targets, for head and neck cancer and for lung, the time savings can be even greater.”
As Dr. Mundt indicates, the advantages of speed correlate more to patient comfort than to better outcomes.
“Improving the delivery of treatment is not necessarily associated with better outcomes because you can spare tissues very well with conventional IMRT,” he said. “However, even if you have the same sparing [of organs at risk], I would opt for the speed to make the treatment better quality. The longer a patient is on the table, the more you will have problems immobilizing the patient for accurate treatment delivery. You want to get the patient on and off the table in the shortest amount of time to provide a better quality treatment.”
Advantages of throughput
The shorter treatment times also improve throughput, said Dr. Mundt, adding that there are several advantages to increased throughput. First, the less time the patient is on the table, the less discomfort the patient experiences and the lower the potential for movement (Figure 2). Second, from a hospital administrative standpoint, throughput is crucial for running an effective clinic. This may in turn enable the clinic to treat more patients per day.
“When treating the majority of your patients with VMAT, there can be an increase in throughput,” noted Koren Smith, MS, DABR, Medical Physicist, Johns Hopkins University School of Medicine, Department of Radiation Oncology and Molecular Radiation Sciences, where patients are treated on both Elekta’s VMAT system and the TomoTherapy by Accuray Inc. (Sunnyvale, CA).
Similarly, at UCSD Moores Cancer Center, where RapidArc and TrueBeam are employed, clinicians are treating 40 to 50 patients per single linac per day. “It has significantly increased our patient throughput,” said Dr. Mundt.
The role of helical tomotherapy
Helical therapy technology has been available since 1993, when Mackie et al developed a rotating fan-beam technique using a dedicated helical tomotherapy system.5-6 Today, however, the faster delivery speeds of rIMRT systems may have outpaced the slower treatments helical tomotherapy provides.
Nonetheless, many clinicians believe the better dose distribution and quality treatment plans achieved with tomotherapy outweigh faster treatment times. “The high conformality of the radiation dose with respect to the risk to critical organs is one of the advantages of using tomotherapy. It avoids critical structures very well while hitting the target,” said Dr. Matthew West, Chief Physicist at Tulsa Cancer Institute, Tulsa, OK, who has over 10 years of experience working on TomoTherapy systems.
A recently published study comparing rIMRT to cIMRT and tomotherapy, showed rIMRT and tomotherapy were both advantageous with respect to OAR sparing and treatment delivery efficiency, at the cost of higher dose delivered to normal tissues.1
These results align with the results found by clinicians at Johns Hopkins University School of Medicine, where approximately 20% to 25% of patients are treated on VMAT or TomoTherapy systems. “We have done planning studies on VMAT and TomoTherapy, and they are comparable. The planning objectives are met on both types of plans and while small differences can be seen, there are not major differences,” said Smith.
The average ‘beam on’ time for VMAT when treating the prostate or pancreas, using a single-arc, and conventional fractionation, such as a 1.8Gy to 2Gy fraction size, is < 2 minutes, indicates Smith. On TomoTherapy, however, the beam-on time for a typical prostate patient is 2 to 4 minutes. Yet Smith considers the treatment times on TomoTherapy to be very reasonable.
“TomoTherapy is very effective, and it is not an outdated technology. In a lot of planning comparisons, it can deliver more homogenous dose to the target while sparing critical structures more than other types of delivery,” Smith reported.
While there have been several technical advances in rIMRT systems, helical tomotherapy has recently undergone a system overhaul. In October 2012, Accuray Inc. launched its new TomoTherapy H Series, including the TomoHDA System, designed with faster planning, faster delivery, and increased quality. Some of the key features of the TomoHDA system include TomoEDGE Dynamic Jaws technology, designed to provide added flexibility in treatment delivery by sharpening dose fall off and accuracy.
“The advantage of TomoTherapy with respect to OAR is the high conformality, especially with TomoEdge or dynamic jaws. The efficiencies arise from the TomoTherapy process. Dose falls off much faster in a superior and inferior direction than it used to, and it also provides much tighter dose distribution,” West pointed out.
Wiezorek et al also concluded that the overall treatment plan quality using tomotherapy seemed better than the other treatment planning technologies.1
According to the lead author of the study, Tilo Wiezorek, PhD, Department of Radiation Oncology, University of Jena, Jena, Germany, the advantage to tomotherapy is a higher degree of freedom compared to VMAT techniques or fixed-beam IMRT. However, he added, “A fixed-beam IMRT plan with a mixture of high photon energy (eg, 15MV) and lower energy (eg, 6MV) in combination with a preoptimized beam-angle setup very often offers better dose distributions for PTVs with a strong asymmetric position in the body and for high-weight patients, too. Especially for retreatments of patients with previous dose impact this offers a better choice,” said Dr. Wiezorek.
Recent improvements to the TomoTherapy system may give it an edge when it comes to accuracy and even speed. New TomoEDGE Dynamic Jaws technology combined with VoLO Planning, a graphics processing unit (GPU)-based treatment planning solution, enables high-speed parallel processing for both dose calculation and optimization. VoLO leverages advanced graphics processing technology and a new calculation algorithm to significantly reduce treatment-planning times and add flexibility in developing even very complex radiation therapy plans.
“VoLO has sped up the time it takes to turn around a treatment plan,” said West. “On the older system without VoLO, before we even started planning, it could take between 30 minutes and 4 hours, depending on how complicated the case was. Now with VoLO it only takes 2 minutes before we start planning.”
He continued, “When you look at the efficiencies, the system is very simple. Unlike a conventional accelerator, there are no ancillary components or special modes for special types of treatments, so whether you’re planning a prostate, brain, breast or stereotactic case, you plan it and treat them the same. The efficiencies come in terms of ease of workflow and safety.”
“The simplified process—no machine treatment aids, no transfer of planning data—allow dosimetry to utilize the same general planning approach independent of treatment type. The therapists can focus on the patient and their setup. The treatment data isn’t transferred from one computer to another, but is verified by physics prior to treatment. Ultimately, this attention to patient setup and image guidance allows clinicians to reduce treatment margins and minimize dose to critical structures,” said West.
The dose factor
Since the goal of radiation therapy is to administer a therapeutic dose of radiation to a target while limiting the side effects caused by delivering the dose to surrounding tissues and vital organs, there is an ongoing pursuit in radiotherapy to achieve an optimal dose distribution.
The trend to lower radiation exposure to patients has been reinforced by industry organizations, such as MITA, The American Association of Physicists in Medicine (AAPM), the Alliance for Radiation Safety in Pediatric Imaging, and Image Wisely. Therefore, radiation dose is another important consideration when comparing rIMRT to cIMRT and helical tomotherapy.
The perceived benefit of the VMAT radiotherapy delivery technique over IMRT is a reduction in delivery time, but VMAT also uses fewer monitor units (MU), resulting in a lower patient total body dose. A study comparing the delivery efficiency and time for the IMRT and VMAT plans for a series of prostate cases found VMAT plans resulted in a statistically significant reduction in the rectal V25Gy parameter of 8.2% on average over the IMRT plans.7 These reductions in rectal dose were achieved using 18.6% fewer MU and a delivery time reduction of up to 69%.7 Therefore, in addition to speed, the lower cumulative MU of the VMAT system is important for patient safety because it reduces the overall amount of radiation.
“A secondary advantage of VMAT with respect to cIMRT is that VMAT units require less MU, which is a measure of how much radiation is produced by the accelerator. Fewer MU means lower amounts of leakage dose outside of the treatment field. The patient receives lower doses out of field, which corresponds to a theoretical reduction to treatment related cancers. It is like the ALARA principle,” indicated Fontenot.
Lowering radiation to patients is not exclusive to rIMRT. Although conventional MU verification calculations are not applicable to TomoTherapy treatments,8 Fontenot points out that helical tomotherapy delivers highly conformal dose distributions.
“Tomotherapy utilizes a similar delivery approach and delivers highly conformal dose distributions, which lets us deliver a very high dose of radiation to the target, and a very low dose of radiation to the surrounding critical structures. Tomotherapy relies on treating the tumor from several different directions, which involves irradiating larger volumes of normal tissue albeit at much lower doses,” said Fontenot.
“When you’re comparing VMAT and tomotherapy on the basis of low dose volumes, we’ve had studies indicating that there are some tradeoffs. The intermediate dose range on tomotherapy is a little better, and VMAT is a little better in the low to very-low dose range.”
Fontenot says the jury is still out on which one is better at sparing normal tissue at low to intermediate doses, and how those differences translate into risks of secondary cancers.
Is it a tie?
With so many variables involved in radiation therapy, Dr. Wiezorek is reluctant to declare a winner.
“From my point of view, we cannot proclaim a principle advantage of rIMRT versus cIMRT,” said Dr. Wiezorek.
While in many cases the reduced delivery times on rIMRT offer a significant advantage, this time advantage may be limited in some complex cases.
“Rotational techniques offer faster treatments for low complex targets, such as prostate cancer, or high complex and symmetrical PTVs, like head and neck with 3 dose levels. However, for high complex and symmetrical PTVs, rIMRT is faster only if TomoTherapy is used or only if a maximum of 2 arcs are used for VMAT. If some regions have to be blocked, rotational techniques do not significantly speed up the treatment,” said Dr. Wiezorek.
However, with recent advances in rIMRT systems and tomotherapy technology, these techniques may soon outperform cIMRT in both speed and accuracy.
References
- Wiezorek T, Brachwitz T, Georg D. Rotational IMRT techniques compared to fixed gantry IMRT and tomotherapy: Multi-institutional planning study for head-and-neck cases. Radiat Oncol. 2011;6:20.
- Otto K. Volumetric modulated arc therapy: IMRT in a single gantry arc. Med Phys. 2008;35: 310-317.
- Varian TrueBeam – Flattening-Filter-Free Mode. http://sudentas.com/physics/varian-truebeam/flattening-filter-free/. Accessed August 7, 2013.
- Wang JZ, Rice R, Mundt AJ, et al. Feasibility and advantages of using flattening filter-free mode for radiosurgery of multiple brain lesions. Pract Rad Onc. 2012;2, e165-e171.
- Mackie TR, Holmes T, Swerdloff S, et al. Tomotherapy: A new concept for the delivery of dynamic conformal radiotherapy. Med Phys. 1993;20: 1709-1719.
- Zuang T, Huang L, Qi P, Yu J. Radiation therapy: Clinical application of volumetric modulated arc therapy. App Rad Onc. 2013;2.
- Hardcastle N, Tome WA, Foo K, Et al. Comparison of prostate IMRT and VMAT biologically optimised treatment plans. Med Dosim. 2011;36:292-298.
- Gibbons JP, Smith K, Cheek D, Rosen I. Independent calculation of dose from a helical TomoTherapy unit. J App Clin Med Phys. 2009;10:1.
