Immunotherapy After Surgery Helps High-Risk Bladder Cancer Patients Live Cancer Free Longer
 Results from a large clinical trial, known as AMBASSADOR, show that treatment with an immunotherapy drug may nearly double the length of time people with high-risk, muscle-invasive bladder cancer are cancer-free following surgical removal of the bladder. The study, published in the New England Journal of Medicine and led by researchers at the National Institutes of Health, found that postsurgical treatment with pembrolizumab (Keytruda), which is approved by the FDA for treating at least 18 different cancers, was superior compared with observation.
Results from a large clinical trial, known as AMBASSADOR, show that treatment with an immunotherapy drug may nearly double the length of time people with high-risk, muscle-invasive bladder cancer are cancer-free following surgical removal of the bladder. The study, published in the New England Journal of Medicine and led by researchers at the National Institutes of Health, found that postsurgical treatment with pembrolizumab (Keytruda), which is approved by the FDA for treating at least 18 different cancers, was superior compared with observation.
“This study shows that pembrolizumab can offer patients another treatment option to help keep their disease from coming back,” said lead investigator Andrea B. Apolo, MD, of NIH’s National Cancer Institute (NCI) Research, Center for Cancer Research. “Extending the time that these patients are cancer-free makes a big difference in their quality of life.”
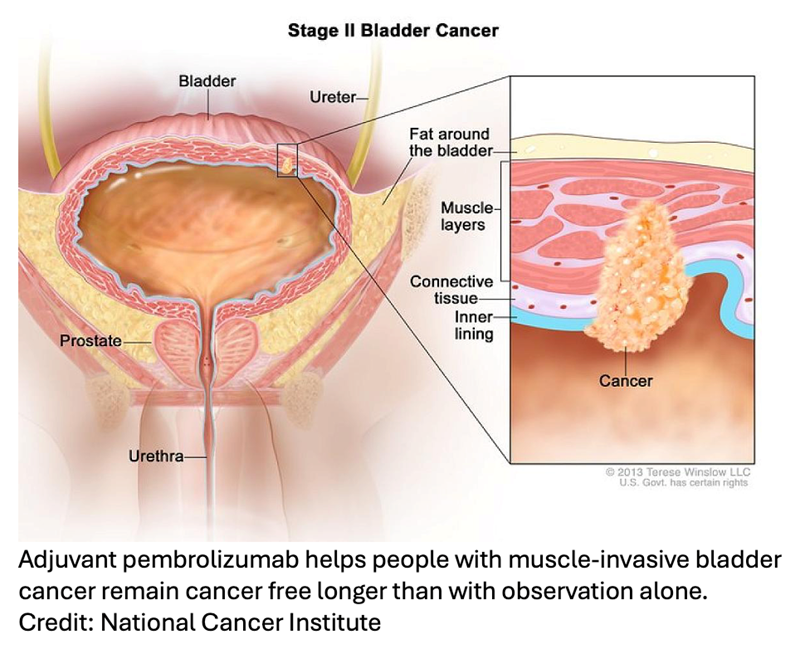
A diagnosis of muscle-invasive bladder cancer means the tumor in the bladder has invaded into and through the muscular layer of tissue that encases the bladder. The standard treatment for this form of bladder cancer is to surgically remove the entire bladder. To improve the chances of successful surgery and of eliminating any cancer cells that may have already escaped from the tumor, patients are given cisplatin-based chemotherapy for a period before surgery, known as neoadjuvant therapy, or after surgery, known as adjuvant therapy.
However, many people with muscle-invasive bladder cancer can’t take or refuse neoadjuvant chemotherapy with cisplatin. Others can’t tolerate adjuvant cisplatin-based chemotherapy. Still others, who despite having received neoadjuvant chemotherapy with cisplatin, have persistent muscle-invasive disease but can’t be treated again with adjuvant cisplatin-based chemotherapy. Historically, these groups of patients were instead carefully monitored to watch for signs of relapse.
As an alternative to observation, researchers have been investigating giving patients immunotherapy drugs after surgery to see if it can help them live longer without their cancer coming back.
In 2021, FDA approved nivolumab (Opdivo) as an adjuvant therapy for people with high-risk, muscle-invasive bladder cancer after a clinical trial showed that this immune checkpoint inhibitor — a type of immunotherapy that releases the brakes of T cells so they can recognize and attack tumors—doubled the median length of time patients remained cancer-free compared with a placebo. Adjuvant nivolumab is now the standard of care in this setting.
In the current trial, researchers investigated whether the immune checkpoint inhibitor pembrolizumab would also be effective as an adjuvant treatment. They randomly assigned 702 patients with high-risk, muscle-invasive bladder cancer who had undergone bladder-removal surgery to receive adjuvant therapy with pembrolizumab every three weeks for a year, or to observation for the same period of time. About two-thirds of the patients in the trial had completed neoadjuvant therapy with cisplatin.
After a median follow-up of almost four years, patients in the pembrolizumab group remained cancer-free for a median of 29.6 months, compared with 14.2 months for the observation group. Pembrolizumab was well tolerated, with the most common side effects being fatigue, itching, diarrhea, and an underactive thyroid.
In some cancer types, immune checkpoint inhibitors such as pembrolizumab are more effective against tumors that are PD-L1-positive —that is, the tumor cells produce a large amount of the PD-L1 protein on their surface, than those that don’t, or PD-L1 negative. So Dr Apolo and her colleagues assessed whether the effect of pembrolizumab varied by PD-L1 status.
Among the 404 patients whose tumors were PD-L1-positive, those treated with pembrolizumab remained cancer free for a median of 36.9 months, compared with 21 months for those in the observation group. Among the 298 patients whose tumors were PD-L1-negative, those treated with pembrolizumab remained cancer free for a median of 17.3 months, compared with nine months for the observation group. The researchers concluded that PD-L1 status should not be used to select patients for treatment with pembrolizumab, as both groups benefited from adjuvant pembrolizumab.
In preliminary data on overall survival, at three years, about 61% of patients in the pembrolizumab group were still alive, compared with about 62% of patients in the observation group. The researchers pointed out that many patients in the observation group began taking nivolumab once it was approved or withdrew from the study, which may have skewed the results and made the overall survival data difficult to interpret.
Research teams are already building on the study’s findings by exploring adjuvant treatment using various combinations of drugs with immune checkpoint inhibitors. Researchers are also testing biomarkers to identify patients with high-risk, muscle-invasive bladder cancer who could benefit most from adjuvant treatment of any kind and spare those who may not need it.