Trends, trials and developments in radiation therapy for esophageal cancer
Images
Although only 1% of cancers diagnosed in the United States are esophageal cancer, patients with this disease often face a poor prognosis. According to the American Cancer Society, approximately 20% of patients survive more than 5 years after diagnosis.1
Of the 2 major types of esophagus cancer—squamous cell and adenocarcinoma—the former has historically accounted for 75% of esophageal cancers in the United States, with incidence rates for esophageal adenocarcinoma on the rise. One study reports average annual percentage increases of 6.1% in men and 5.9% in women.2
Outside of the United States, esophageal cancer is more prevalent, with the highest incidence rates in Asia and Africa. The World Cancer Research Fund International reports that about 81% of esophageal cancer cases occur in less developed countries.3
“In the U.S. where new technology is quickly adopted, esophageal cancer is not very common, so we have a limitation in conducting trials—accruing patients and collecting data,” says Michael Rutenberg, MD, PhD, assistant professor in the Department of Radiation Oncology at the University of Florida Proton Therapy Institute. This presents a troubling dichotomy: Advanced technology that could benefit most esophageal cancer patients is not available where incidence rates are highest.
“Landmark studies for esophageal cancer only come every few decades, so there are no landmark studies to support novel technology such as proton therapy,” Dr. Rutenberg says. “When we moved from the 3D conformal radiotherapy [3DCRT] era to the [intensity-modulated radiation therapy] IMRT era, the best support for the new technology came not from prospective trials, but from large retrospective cohort comparisons.”
Surgery vs. Radiation
One 1992 landmark study by Herskovic et al, however, changed the role of using radiation therapy (RT) for treating esophageal cancer.4 “Prior to this study, it was believed that the only curative therapy for esophageal cancer was surgery,” says Michael G. Haddock, MD, professor of radiation oncology, Mayo Clinic College of Medicine, and a consultant and chair of the Clinical Practice Committee, Department of Radiation Oncology. At that time, RT was a 2-dimensional treatment—anterior-posterior/posterior-anterior (AP/PA) with lateral and oblique fields that gave adequate dose to the tumor but high doses to the heart and lungs. Today, radiation therapy is indicated for patients with locally advanced esophageal cancer that has penetrated the muscular lining or when regional lymph nodes are involved. It may also be indicated for palliative care in metastatic cancer cases. For many patients, treatment involves a trimodality approach of chemotherapy, radiation, and surgery.
Yet, in cases of locally advanced esophageal cancer, the issue remains when, or if, the patient should undergo surgery. “It is a question of whether there is a pathological complete response to radiation and chemotherapy,” Dr. Haddock explains, noting that only about 25 percent of patients who undergo radiation and chemotherapy without surgery are cured. “There is no reliable test to definitively indicate complete response short of surgical resection. We can put off surgery until there is progression of the disease, but then complications increase.”
While local control improves with the addition of resection, survival is less certain, says Dr. Haddock. Additionally, some patients with early stage disease show excellent survival following radiation and chemotherapy without resection.
While surgery remains under debate, confusion regarding use of preoperative radiation has been lifted, says Dr. Rutenberg. “The CROSS [ChemoRadiotherapy for Oesophageal cancer followed by Surgery Study] Trial is perhaps the most important study for esophageal cancer treatment in the last 10-plus years,” he says. “While it doesn’t support any single type of equipment or technology, it solidly ended the debate on the importance of pre-operative radiation in the management of esophageal cancers.”
Motion Issues and Organ Sparing
The standard of care also involves accounting for motion. At MD Anderson Cancer Center, Stephen G. Chun, MD, assistant professor, Department of Radiation Oncology, Division of Radiation Oncology, uses a 4-dimensional (4D) respiratory-gated scan to account for motion in treatment planning. He also uses deep-inspiration breath holds when appropriate.
As technology has evolved, so have treatments. RT for esophageal cancer migrated to more advanced techniques such as 3DCRT followed by IMRT. In 2017, a large single-institution cohort study conducted at MD Anderson Cancer Center on the long-term outcomes of treatment with IMRT for esophageal cancer found that IMRT improved organ-sparing effects, demonstrating excellent toxicity and survival outcomes compared with 3DCRT. The authors concluded that IMRT should be considered for photon-based treatments.5
“With IMRT, there is the ability to achieve dramatically better sparing of radiation doses to the heart and lungs compared with 3D techniques,” says Dr. Chun. “With volumetric arc IMRT [VMAT], we are able to get very good plans with substantially shorter treatments than static beam arrangements.”
Whether a site uses IMRT or VMAT largely depends on the treatment plan. Dr. Rutenberg often starts with a VMAT plan for esophageal cancers; however, he also evaluates an IMRT plan and selects what’s best for individual patients. “We can now focus on the nuances of radiation therapy and perhaps focus on quality of life and reduction in complications,” he says. “However, what we do in radiation therapy is contingent on systemic disease control to help improve long-term patient outcomes.”
The key consideration in any radiation plan is avoiding critical structures, adds Dr. Haddock. “Recent studies suggest that the outcomes for cancers in the mediastinum are tied to heart and lung dose,” he says. “Lower doses to the heart and lung are associated with increased survival, suggesting that the techniques that spare the heart and lung are beneficial.”
Proton Therapy
As for the role of proton therapy for treating esophageal cancer, MD Anderson was the first institution to prospectively compare proton therapy with IMRT for stage III or locally advanced esophageal cancer. A 2012 study found few severe toxicities with encouraging pathologic response and clinical outcomes at 20-month follow-up with proton therapy.6
“Proton therapy has the ability to further reduce dose to heart and lungs, and that might provide additional benefit for patients,” notes Dr. Chun, who has enrolled patients in the randomized phase II trial (open as of press time) comparing IMRT and protons for esophageal cancer,
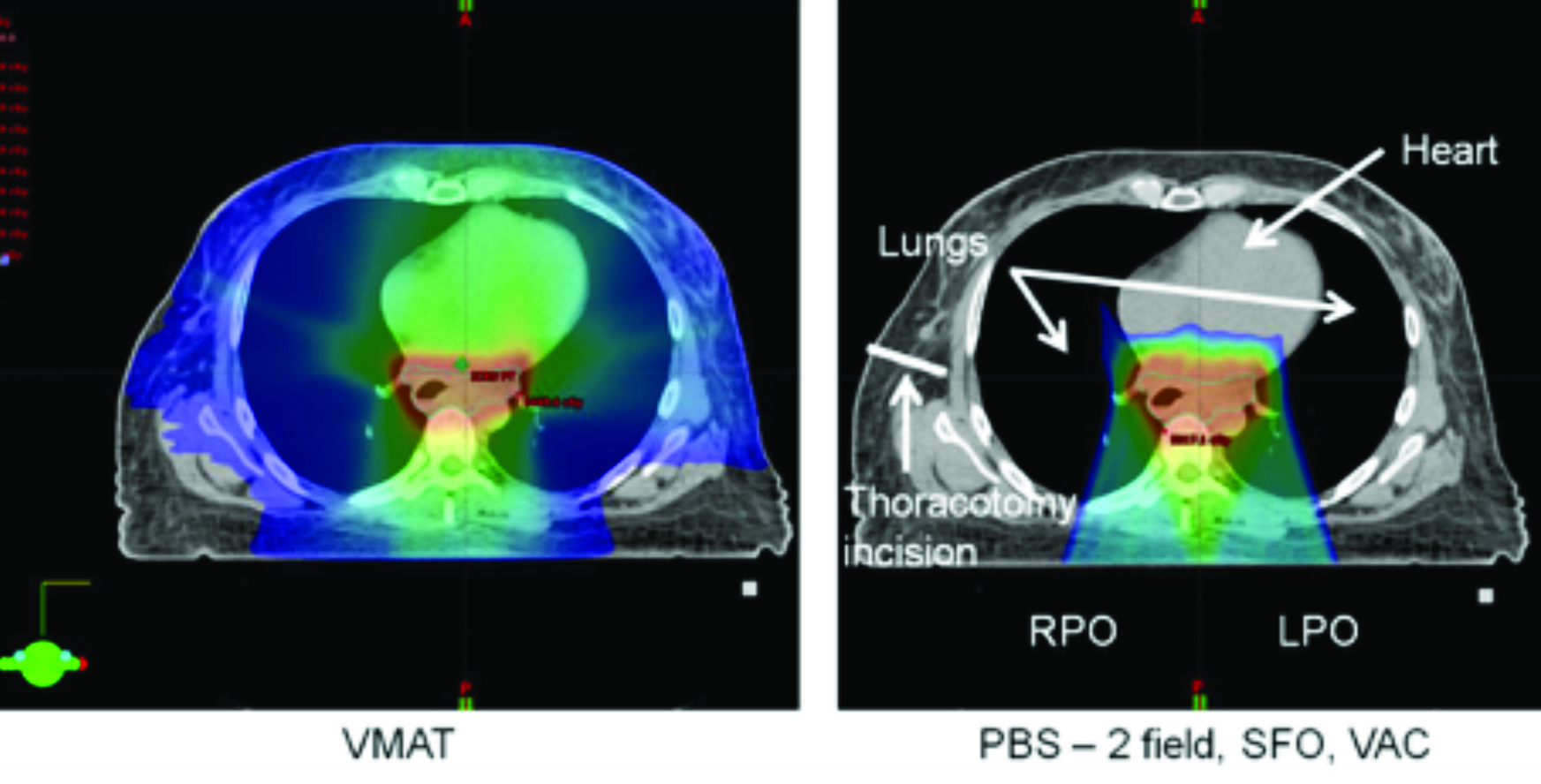
Both Drs. Haddock and Rutenberg also agree that proton therapy shows promise in treating esophageal cancer and, in particular, sparing the heart and lung (Figure 1). “Protons will have a really important role in future treatments,” says Dr. Rutenberg, noting that the University of Florida Proton Therapy Institute has treated roughly 20 esophageal cancer patients with protons. While patient volumes are limited due to lack of third-party payor reimbursement for proton therapy, this could change as results from clinical trials emerge. For instance, a 3-site study by the Mayo Clinic, MD Anderson and the University of Maryland that retrospectively compared 3D conformal therapy, IMRT and proton therapy found decreased pulmonary, cardiac and wound complications in patients treated with advanced techniques.7 Additionally, a randomized study comparing IMRT to proton therapy is expected to open for enrollment through the NRG Oncology cooperative group later this year, notes Dr. Haddock.
“Of all the disease sites where protons might benefit patients by sparing the heart and lungs, esophageal cancer is on the top of that list,” he says.
Related Issues and Considerations
Several additional hot-button issues surround RT for esophageal cancer, including treating cancers in the lower esophagus, known as the gastroesophageal junction. The European standard of care is perioperative chemotherapy—chemotherapy before and after surgery—while the U.S. standard is chemoradiation before surgery.
“These 2 treatment paradigms haven’t been compared head to head for esophageal cancer,” Dr. Chun explains. “Although the CRITICS [ChemoRadiotherapy after Induction Chemotherapy in Cancer of the Stomach] trial in Europe compared perioperative chemotherapy against adjuvant chemoradiotherapy after surgery, this was mostly for gastric cancer. This is an area that could potentially be studied further in esophageal cancer.”
In the CRITICS trial, the authors reported that overall survival was not improved with postoperative chemoradiotherapy compared with postoperative chemotherapy when patients received adequate preoperative chemotherapy and surgery. They suggest that future studies evaluate preoperative treatments.8
Oligometastatic disease, an intermediate state of metastasis between localized disease and widespread metastasis, is another concern. The disease was first proposed in 1995 by University of Chicago Medicine physicians Samuel Hellman, MD, FASCO, and Ralph R. Weichselbaum, MD. They hypothesized that some patients in this intermediate state could respond to a curative therapeutic strategy by treating limited metastatic sites with surgery or radiation. They confirmed their hypothesis in a study on oligometastatic colorectal cancer published in May 2018.9
Genetics may also factor in to esophageal cancer treatment, as a small percentage of patients with esophageal cancer have the HER-2 gene receptor, the same gene found in some aggressive forms of breast cancer, says Dr. Chun,“We can potentially use a genetic test for the HER-2 receptor, especially in patients with metastatic disease, and if positive, they could be targeted with Herceptin or other treatment drugs,” he adds.
While outcomes are not great for locally advanced esophageal cancers, some studies are examining immunotherapy and checkpoint inhibitors in combination with radiation therapy with promising response rates, says Dr. Chun.
“I’m hopeful that immunotherapy can be incorporated if it is shown to improve patient outcomes to move the ball forward for this increasingly common cancer,” he says.
References
- American Cancer Society. https://www.cancer.org/cancer/esophagus-cancer/about/key-statistics.html. Accessed August 22, 2018.
- Hur C, Miller M, Kong CY, et al. Trends in esophageal adenocarcinoma incidence and mortality. Cancer. 2013;119(6):1149-1158.
- World Cancer Research Fund International. https://www.wcrf.org/int/cancer-facts-figures/data-specific-cancers/oesophageal-cancer-statistics. Accessed August 22, 2018.
- Herskovic A, Martz K, Al-Sarraf M, et al. Combined chemotherapy and radiotherapy compared with radiotherapy alone in patients with cancer of the esophagus. N Engl J Med. 1992;326:1593-1598.
- Shi A, Liao Z, Allen PK, et al. Long-term survival and toxicity outcomes of intensity modulated radiation therapy for the treatment of esophageal cancer: a large single-institutional cohort study. Adv Radiat Oncol. 2017;2(3):316-332.
- Lin SH, Komaki R, Liao Z, et al. Proton beam therapy and concurrent chemotherapy for esophageal cancer. Int J Radiat Oncol Biol Phys. 2012; 83(3):e345-e351.
- Lin SH, Merrell KW, Shen J, et al. Multi-institutional analysis of radiation modality use and postoperative outcomes of neoadjuvant chemoradiation for esophageal cancer. Radiother Oncol. 2017;123(3):376-381.
- Cats A, Jansen EPM, van Grieken NCT, et al. Chemotherapy versus chemoradiotherapy after surgery and preoperative chemotherapy for resectable gastric cancer (CRITICS): an international, open-label, randomised phase 3 trial. Lancet Oncol. 2018;19(5):616-628.
- Pitroda SP, Khodarev NN, Huang L, et al. Integrated molecular subtyping defines a curable oligometastatic state in colorectal liver metastasis. Nature Com. 2018; 9:1793.
Citation
MB M. Trends, trials and developments in radiation therapy for esophageal cancer. Appl Radiat Oncol. 2018;(3):49-51.
September 22, 2018